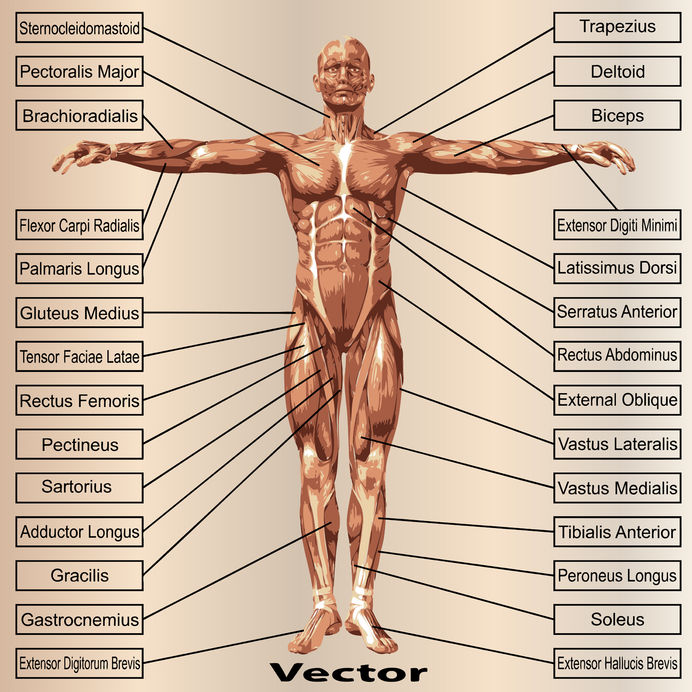
The following describes various injuries and syndromes common to fitness practitioners. While this information can be useful in determining appropriate first aid or symptomatic relief methods, it is important to be aware of the distinction between first aid and relief of symptoms versus diagnosis and treatment.
A single symptom (such as lower back pain) can have a variety of causes, which are not immediately obvious and can require diagnosis by a physician or certified therapist that can prescribe treatment.
Do not to use the information below to “self-diagnose;” use it only as guidelines for appropriate first aid or symptomatic relief or, to see a physician.
Exercise professionals are admonished to refrain from the process of diagnosis and/or prescription of treatment or rehabilitative exercise. We encourage such to use RICE and for the affected person to visit their doctor. (RICE is an acronym for Rest, Ice, Compression, and Elevation.)
Statements such as “that sounds like chondromalacia – why don’t you try strengthening the medial quad to help out” or “you’ve got low back syndrome” involve a judgment that can be construed in a court of law as a diagnosis and/or prescription of rehabilitative exercise.
Common exercise injuries
Overuse Injuries
The heading of overuse injuries is generally broad. It can include a vast majority of exercise-related injuries. Generally overuse injuries are chronic ones, meaning that no single event causes them (as with a sprained ankle or a broken leg), but repetitive motion with time, i.e., months or years of training, gradually weaken or irritate the area in question until exercise becomes difficult or impossible or other symptoms appear.
The vast majority of overuse injuries can be avoided by proper attention to form and technique, appropriate rest, proper equipment (especially footwear), and gradual increase of exercise frequency, intensity, or duration. Rest is critical during training, when feeling any irritation other than muscle soreness.
The best cure for overuse injuries are: rest followed by a gradual return to activity, coupled with an awareness of the problem activity, and appropriate corrective measures. This could a gradual return to exercise, appropriate strengthening, or avoiding specific activities or exercises.
Patellofemoral Syndrome (“Runner’s Knee”) / Chondromalacia
Chondromalacia literally refers to the wearing away of the cartilage on the back surface of the kneecap, which might be first exhibited as a “clicking” or “grating” sound, and knee pain under the patella (kneecap).
Chondromalacia refers to the condition, and not a specific disease state, as a great many possible causes exists for damage to the cartilage.
Patellofemoral syndrome, likewise, refers to generalized knee pain, often associated with runners, but not limited to runners alone. In this context, the cause is usually improper running mechanics over a period of time and in many cases, the cause is unknown. The precursor to patellofemeral syndrome can be patella maltracking that can occur from several different causes.
Once chondromalacia has occurred, the process is irreversible, and attention is paid to achieving the maximal amount of pain-free activity, and avoiding activities which will cause further damage to the joint. Keeping the muscles surrounding the knee strong becomes crucial as it relieves the demand off or from as lay persons like to say it, the knee joint.
Note that patellofemoral pain is of a more general nature, and may or may not be due to the pathological condition of chondromalacia.
It is best to consult a physician or a physical therapist when any sort of knee pain is encountered.
Plantar Fasciitis and Neuromas
Plantar fasciitis is literally an inflammation of the plantar fascia, a web of tough, fibrous connective tissue on the bottom of the foot. Neuromas are irritated nerve endings, but can cause pain in the foot (or other places, depending on the nerve in question). Distance runners and walkers are often affected by Plantar Fascitis.
Either of these conditions should be examined by a doctor. While both are commonly caused by overuse, the question of whether the condition is due to poor technique, simple overuse, or an orthopedic problem should be determined. In this way, you can address the problem and avoid a reoccurance.
In the case of the latter, orthotics (inserts for shoes designed to help maintain proper impact cushioning and support for the foot) can play a major role in the prevention of future episodes.
Lateral Epicondylitis (“Tennis elbow”) and the more general Tendonitis/Arthritis/Bursitis
Any “-itis” condition refers to inflammation or irritation. In the cases of tendonitis, arthritis, and bursitis, sites of inflammation include the tendons, joints, and bursae (fluid-filled sacs provided cushioning between tendons and bones), respectively.
These conditions should involve a referral to your physician. Tendonitis and bursitis are common overuse injuries, andoften go hand in hand. Rehabilitation will generally include rest and enhancing flexibility and strength of all muscles surrounding the joints near the area in question.
Arthritis can be caused by two distinct disease processes – osteoarthritis is essentially “wear and tear” on joints, in which the cartilage covering the articulating surfaces of the bones becomes worn, and the joint reacts, often by swelling and filling with fluid. It can become quite tender, and motion can become difficult.
Rheumatoid arthritis is an autoimmune disorder in which the body launches an attack on its own joint tissues. While much less common than osteoarthritis, it can be severely debilitating.
Rehabilitation for arthritis generally involves activities that are low-impact in nature, and strengthening exercises. Activities are carried out through a “pain-free range of motion” (ROM limited by the onset of discomfort), and no activity is recommended during periods of active inflammation.
Shin Splints and Compartment Syndromes
Shin splints are a common name for pain felt in the anterior portion of the calf, which can be due to a variety of causes, from muscle imbalances to something as serious as a compartment syndrome.
General treatment for shin splints involves RICE, strengthening exercises for supporting muscles surrounding the ankle joint, soft tissue mobilization of the anterior shin muscles, and flexibility exercises. Implementing a calf stretching program may offer relief of symptoms. Orthotics may also be indicated to prevent reoccurance.
Compartment syndromes are a much less common, but more serious problem. This is a condition in which one of the compartments between muscles that contains blood vessels and/or nerves becomes swollen, compressing the blood vessels and/or nerves. It can lead to pain, swelling, and discomfort, and in severe situations, may be an emergency situation requiring surgical intervention.
Common exercise reactions
Some people experience reactions to exercise, ranging from uticaria, a harmless red blotchiness on the neck, face, or arms, to exercise induced asthma or bronchospasm, to anaphylaxis.
Exercise-induced asthma (EIA) is most likely to strike individuals exercising in cold, dusty, or excessively humid environments, and can range in severity from mild coughing to severe discomfort. Individuals who suspect that they have exercise-induced asthma are encouraged to see a doctor and to ensure the best possible treatment for the condition.
There is a rare condition, due to allergic reaction, called exercise-induced anaphylaxis. This is a life-threatening situation, and requires immediate medical attention. Any person suspecting that they are prone to EIA should consult with their physician before resuming exercise.
General recommendations for persons with EIA include an extended warm-up, avoidance of cold, dusty, or extremely humid environments for exercise, pursed-lip breathing, and keeping an inhaler handy for use during exercise (if recommended by physician). You may consider wearing a dust or surgeons mask in some situtations.
Physical Therapy
- How Often?
While there are multiple factors, the frequency of physical therapy/massage primarily depends upon the persons size, training intensity, and training frequency. - Massage is used primarily to keep you from injury and over training and can increase flow of nutrients to muscles, reduce tension and stress, increase flexibility, enhance nervous system functions, induce sleep, and increase appetite.
- As a general rule of thumb, the average fitness buff should have a physical therapist check and massage them based on the therapists judgement at least once every 6-8 weeks. Depending on your individual uniqueness, scheduled visits will vary.
- Before seeking a massage, you should first try to combat over training (see Table 1). If you still find slow recovery from soreness and other exercise pains, you should visit your therapist.
- There are two types of massage; local and full body. For high training loads, a full body massage is advisable (twice per week). These massages should not be deep, but relaxing with rubbing and kneading techniques. If training loads are light or medium, a massage once every two weeks is sufficient.
- Local massage is used to treat special areas. An example of a local massage is when you may need extra attention to the hamstrings because of a particular activity that exerts constant work on a specific muscle such as the hamstrings or upper back. When speed-strength training, special attention should be given the lower back, glutes, and hamstrings. A massage should be given only by a qualified sports massage therapist.
- For most athletes, either a local or full massage should be obtained at least once every 3-4 weeks. The harder you train, the more frequent you will need them. Talk to your therapist or ask one of our experts.
- To prevent injury and increase skills requires that proper care be taken with the body. While times of massage can vary, see Tables 2 & 3 for suggested times.
Techniques to combat over training:
- Stop training for one week, a light warm-up and stretching, do not exceed 30 min/day.
- Reduce protein intake to 15% of total calories.
- Increase complex carbohydrates to 70% of total calories.
- Increase antioxidants to 200% of recommended dosage.
- Sleep requirements: minimum of 9 hours/night.
Full body massage time requirements:
Body Weight (lbs) Time Requirement (min.)
135 or less, 40
136-150, 50
151-200, 60
200+, 60+
Local massage time requirements:
Light (5-10 minutes)
Medium (10-25 minutes)
Hard (20-25 minutes)